Healthcare automation software has become essential for protecting revenue and improving operational stability as organizations face rising administrative pressure, tighter margins, and increasing regulatory scrutiny.
CureAR simplifies automation by structuring complex billing workflows into clear, intelligent processes.
This blog explains how automation works across the revenue cycle, compares manual systems with digital solutions, and shows how practices can improve financial performance through smarter technology.
Why Healthcare Automation Is No Longer Optional
Healthcare automation has become a necessity because:
- Administrative complexity continuously strains healthcare systems
- Billing rules constantly evolve
- Documentation requirements expand
- Payer policies shift frequently
According to the American Medical Association, physicians and their staff spend an estimated 15.1 hours per physician per week on prior authorizations, claims, and related administrative tasks.
In smaller practices, nearly 20% of claims are denied, and a significant portion are never resubmitted at all. Even minor documentation gaps can lead to denied claims or repayment demands.
For practices managing complex billing workflows, including claim management in general practices, automation reduces reliance on manual processes and increases accuracy.
This shift is not about replacing people. It is about supporting them with structured, reliable systems.
What Is CureAR?
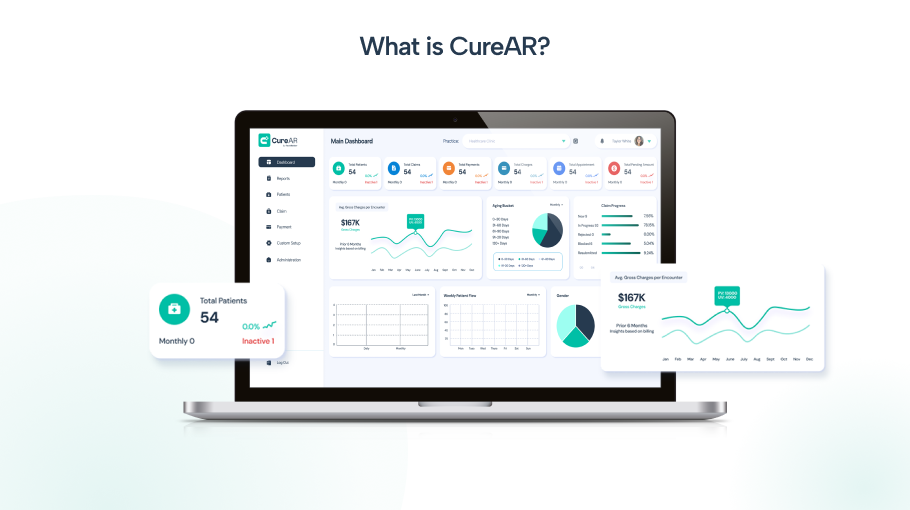
CureAR is an AI-driven medical billing and revenue cycle management platform. It is designed to handle every step of the medical billing process from patient registration and eligibility verification through claim creation, submission, payment posting, denial management, and advanced reporting.
Unlike general billing tools that automate isolated tasks, CureAR is purpose-built as an end-to-end RCM platform.
Every module connects to the next, so data flows consistently across the revenue cycle without manual handoffs or system switching.
Its salient features include:
- HIPAA-compliant
- SOC II certified
- Integrates with 13+ EHR and PMS systems
- Six clearinghouses
- Supports 89+ clinical specialties.
How CureAR Simplifies Key Revenue Cycle Functions
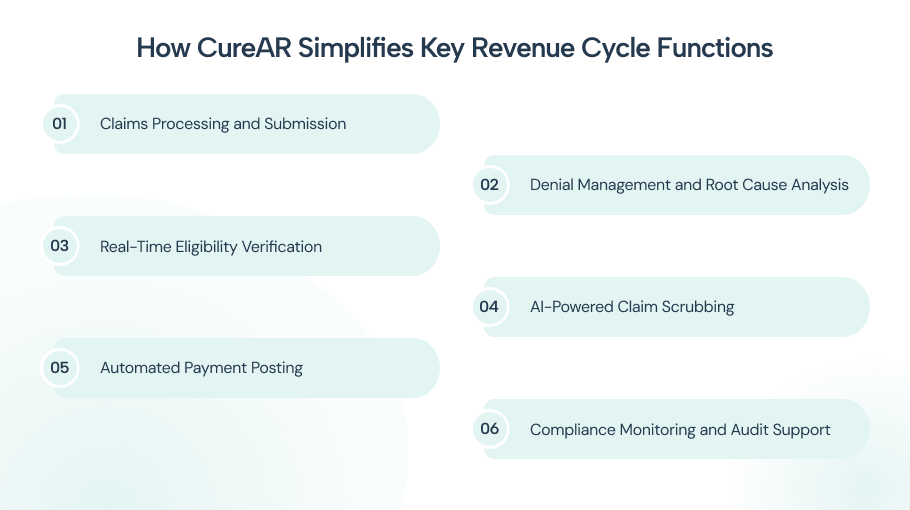
CureAR focuses on simplifying automation across the entire revenue cycle. Each function is structured to reduce risk and increase transparency.
Claims Processing and Submission
Manual claims processing is prone to delays. Staff must verify codes, confirm eligibility, and ensure compliance before submission.
CureAR streamlines this process by:
- Validating coding consistency before submission
- Checking eligibility electronically
- Identifying missing data automatically
The Centers for Medicare and Medicaid Services emphasizes the importance of electronic standards for claims processing under HIPAA transaction requirements.
Automated compliance checks reduce formatting errors and submission rejections. When claims are cleaner at first submission, first pass acceptance rates improve.
Denial Management and Root Cause Analysis
Denials are expensive as physicians spend significant time and resources managing denied claims. CureAR tracks denial patterns and identifies recurring causes.
Instead of reacting after revenue is lost, practices can address root issues proactively. Structured denial analysis reduces repetitive mistakes and strengthens documentation workflows.
Real-Time Eligibility Verification
Insurance eligibility issues are among the most preventable sources of claim denials. CureAR runs real-time and batch eligibility verification through EDI clearinghouse integration before the patient’s appointment, not after the claim is submitted.
This catches coverage mismatches and demographic errors early, before they create downstream billing complications.
AI-Powered Claim Scrubbing
CureAR integrates with Alpha II clinical coding compliance content the same payer-specific rules used by major clearinghouses and enterprise health systems.
Before any claim reaches the clearinghouse, the system checks it against clinical coding requirements, medical necessity criteria, and payer-specific edits.
This catches violations that basic rules engines miss entirely. Practices using CureAR consistently achieve first-pass acceptance rates above 95%.
Automated Payment Posting
Manual payment reconciliation is time-consuming and prone to error. CureAR automates this through Electronic Remittance Advice (ERA) auto-posting, with a manual EOB option for payers that still send paper remittances.
A real-time payments dashboard gives billing teams an immediate view of where collections stand without logging into multiple payer portals.
Denial Management with Root Cause Analysis
Most denial management tools record that a denial happened. CureAR identifies why it happened.
The denial management module includes:
- A denial queue organized by insurance, aging, denial codes, no-response claims, and partial payments
- Open, In-Progress, and Completed workflow tracking with full follow-up history per claim
- AI-driven root cause analysis at the payer, provider, and code level
- Next-action alerts to keep follow-ups on schedule
This allows practices to address the systemic issues driving their denial rates, not just the individual claims sitting in the queue.
Compliance Monitoring and Audit Support
Healthcare billing compliance requires alignment with federal regulations and payer policies. The Office of Inspector General consistently emphasizes documentation integrity and billing compliance as critical safeguards against improper payments.
CureAR supports compliance monitoring through structured documentation validation and audit-ready reporting. Automated oversight reduces the likelihood of errors that trigger external review.
Reporting and Analytics
CureAR’s reporting suite gives billing teams and practice managers visibility across every stage of the revenue cycle. Available report types include charges, payments, adjustments, AR aging, denial trends, occurrence reports, and expected reimbursement forecasts.
All reports export to Excel, PDF, and CSV. Enterprise clients can add Power BI Dashboards for deeper cross-location financial analysis.
Who CureAR Is Built For
Billing complexity varies widely depending on how a practice is structured. CureAR is designed to scale across different operational models without requiring a separate platform at each tier.
Independent Practices
Solo providers and small group practices get access to automated claim scrubbing, real-time eligibility, a denial-tracking dashboard, and EHR integration on the Growth plan.
Onboarding takes 30 days, which is significantly faster than the 90 to 180-day timelines common among other enterprise platforms.
CureAR supports 89+ clinical verticals, making it a strong fit for claim management for general practices as well as specialty-specific billing workflows. Practices see measurable improvement in clean claim rates within the first billing cycle.
Billing Companies and RCM Firms
CureAR is the only platform at its price point offering full white-label capability. Billing companies can brand the platform for their clients and operate it as their own technology infrastructure.
Additional capabilities built specifically for RCM firms include:
- A dedicated RCM Partner Program for firms managing 50 to 300 provider clients
- Portfolio-level analytics across all client accounts
- API access for custom integrations
- Multi-tenant management tools
Multi-Site and Enterprise Organizations
The Enterprise plan supports multi-location management, SSO, HL7/FHIR integrations, custom SLAs, and SLA-guaranteed uptime.
MIPS compliance support is included through Health eFilings, which is a capability not available from any other similar software at a comparable price point. For Medicare-billing practices, MIPS reporting is mandatory, and non-compliance carries direct financial penalties.
Integrations That Eliminate Switching Disruption
A common concern when evaluating new billing technology is disruption to existing clinical workflows. CureAR addresses this directly through its broad integration network.
EHR and PMS Integrations
CureAR connects with 13+ EHR and PMS platforms, including:
- Epic
- AthenaHealth
- eClinicalWorks
- Veradigm
- AdvancedMD
- Tebra
- DrChrono
- WebPT
- CollaborateMD
- eMDs
- inSync
- Office Ally
- CareCloud
Practices do not need to replace their existing clinical system to improve billing performance. CureAR adds the revenue intelligence layer on top of what is already in place.
Clearinghouse Integrations
CureAR connects to six major clearinghouses:
- Office Ally
- Waystar
- SecureConnect
- Change Healthcare
- Availity
- Etactics
Practices keep their existing clearinghouse relationships. CureAR adds the pre-submission optimization layer on top, reducing denial rates without forcing a clearinghouse switch.
Final Thoughts
Healthcare automation software has moved from a competitive advantage to an operational necessity for practices managing complex billing environments.
Manual workflows introduce errors at every stage, and those errors carry a real cost in denied claims, delayed payments, and staff time spent on rework.
CureAR brings automation to each stage of the revenue cycle from eligibility verification and claim scrubbing through denial management, payment posting, and reporting in a single platform that works alongside existing EHR systems rather than replacing them.
Whether you are an independent practice, a billing company, or a multi-site organization, CureAR is built to reduce the friction that costs practices revenue every month.
Frequently Asked Questions
Healthcare automation software uses technology to automate repetitive billing tasks such as claim submission, eligibility verification, payment posting, and denial management.
It reduces errors, speeds up reimbursements, and allows billing teams to focus on work that requires human judgment.
No. CureAR integrates with 13+ EHR and PMS platforms, including Epic, AdvancedMD, AthenaHealth, and Tebra. Clinical workflows stay in place, and CureAR adds the billing intelligence layer on top.
Standard onboarding takes 30 days, including dedicated training for every user role. This is significantly faster than the 90 to 180-day timelines common among enterprise billing platforms.
Yes. CureAR offers full white-label capability and a dedicated RCM Partner Program built for firms managing multiple provider clients, with portfolio-level analytics and API access included.
CureAR connects to six clearinghouses: Office Ally, Waystar, SecureConnect, Change Healthcare, Availity, and Etactics. Practices keep their existing clearinghouse relationships.
Yes. CureAR includes MIPS compliance support through Health eFilings, helping Medicare-billing practices meet mandatory reporting requirements and avoid financial penalties.
Plans start at $129 per month. An outsourced billing model at 3% to 6% of collections is also available, along with annual prepay discounts and multi-provider pricing options.








