Top 10 AI-Enabled Medical Billing Software in USA


What is AI Medical Billing Software?
As the name suggests, AI medical billing software uses artificial intelligence and automation to streamline the revenue cycle from patient registration to claims submission and payment posting. Unlike traditional billing software, AI-driven tools can detect errors, predict denials, automatically correct coding issues, and learn from past data to improve claim accuracy.
In the U.S., adoption of AI-powered billing is accelerating, growing at a CAGR of 24.16% from 2025 to 2030, with most practices already using AI in their revenue cycle operations, and nearly three-quarters adopting some form of automation.
This growth reflects how providers are turning to intelligent software that connects with EHR platforms, uses natural language processing for documentation, and applies predictive analytics to spot revenue leaks before they happen. In short, AI billing software doesn’t just process claims; it thinks, analyzes, and improves them.
10 Best AI Medical Billing Software
These top-rated AI medical billing software are redefining how providers handle claims, payments, and compliance. Each brings intelligent automation to streamline financial performance.

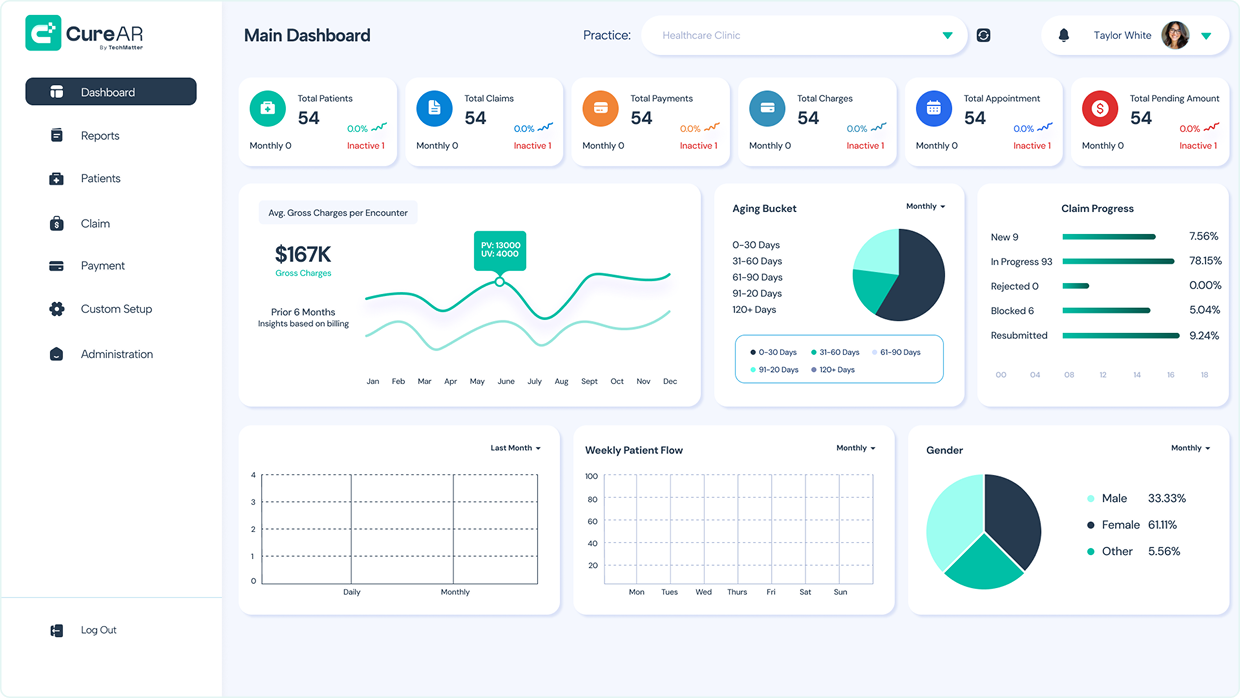
CureAR is a cloud-based medical billing software that uses AI to manage your entire claims process. It carefully reviews claims before submission, focuses on denials, and automatically resubmits corrected claims. With real-time dashboards, you can predict cash flow and spot issues before they lead to revenue losses.
Its predictive analytics help reduce A/R days while ensuring compliance with HIPAA. CureAR stands out by combining extensive industry knowledge with robust automation, resulting in more accurate, efficient billing.
Software Interface
Pros:
- Automates claim scrubbing and validation.
- Real-time dashboards for financial visibility.
- Scalable cloud infrastructure with secure access.
Cons:
- Advanced analytics require training.
- It may be costly for very small practices.
- Requires integration with existing EHR systems.
Features:
- AI-enabled claim scrubbing and validation.
- Real-time denial tracking and auto-resubmission.
- Seamless integration with top EHR systems.
- Predictive analytics for cash flow forecasting.
Why It Stands Out:
- Reduces A/R days by 33% efficiently.
- Enhances billing accuracy and revenue performance.
- Combines AI precision with healthcare expertise.
- Improves staff efficiency and workflow.

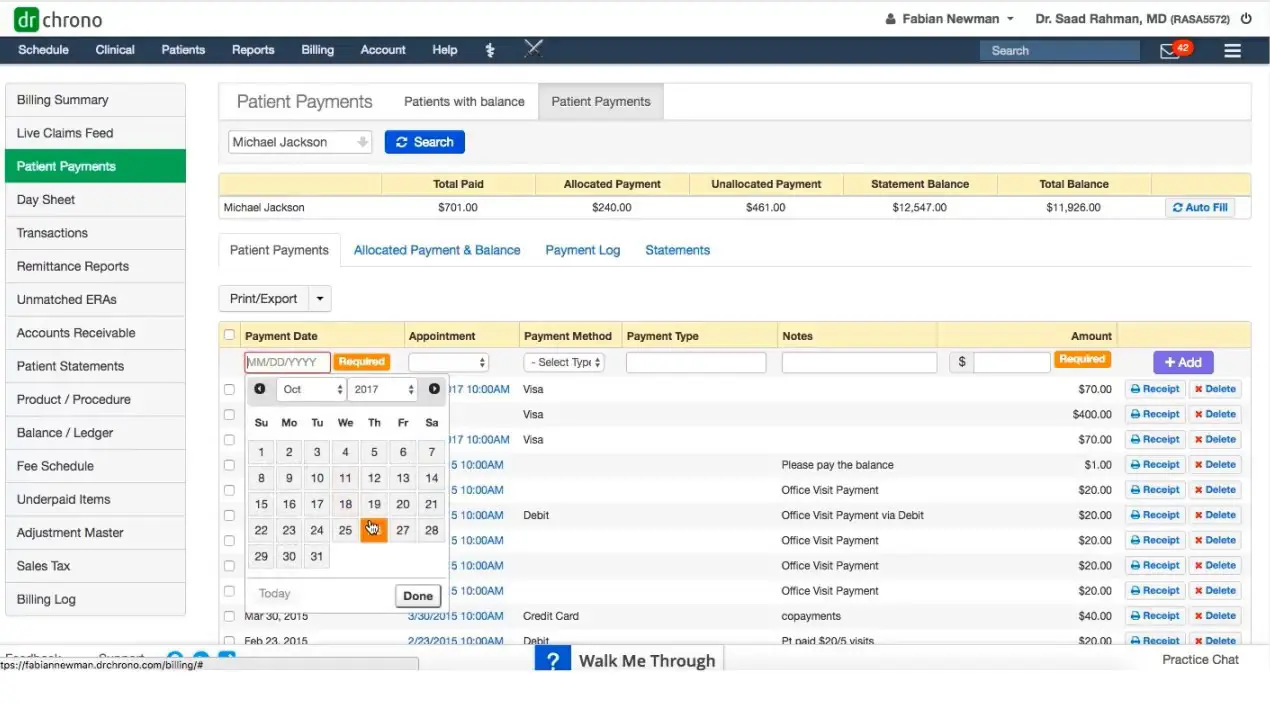
DrChrono offers a complete cloud-based EHR, practice management, and billing system that runs on iPad, iPhone, and web. Their RCM team takes care of everything, from claims to denial resolution, helping providers achieve a clean claim rate of over 96%. With dashboard reporting, practices receive real-time insights into their revenue, denials, and cash flow. DrChrono is designed for flexibility. It supports mobile workflows and allows practices to grow without losing billing accuracy.
Software Interface
Pros:
- 96%+ clean claims improve collections.
- Mobile EHR supports on-the-go workflows.
- Dedicated RCM team reduces staffing needs.
Cons:
- Requires mobile-friendly workflow adoption.
- Onboarding can take significant setup time.
- May lack advanced enterprise analytics.
Features:
- Mobile EHR integrated with billing and coding.
- Transparent BI tools for real-time financial reporting.
- ERA/EOB posting and denial resolution within 48 hours.
Why It Stands Out:
- Mobile-first platform with strong usability.
- AI reduces manual coding effort.
- Great for small and mobile clinics.
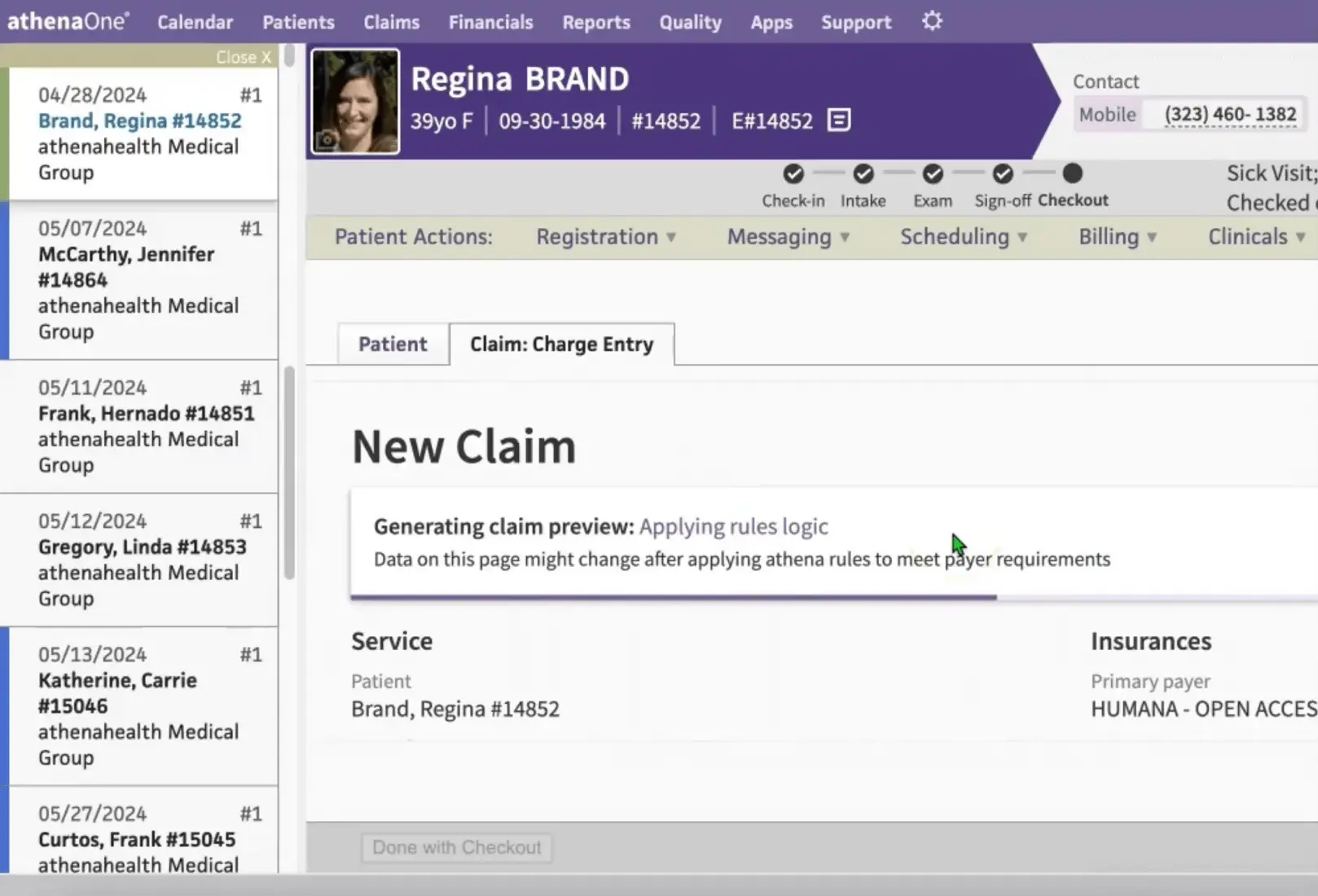
Athenahealth, founded in 1997, is headquartered in Watertown, Massachusetts, with additional offices in Atlanta, Austin, Belfast, and Chennai, India. They serve physician groups, hospitals, outpatient practices, and medical billing professionals across a wide range of specialties. Athenahealth supports both independent practices and large health systems.
Software Interface
Pros:
- Proactively prevents denials with AI.
- Automates prior authorization for speed.
- Ambient AI documentation saves substantial time.
Cons:
- Implementation requires significant time and resources.
- Advanced AI features may need training.
- Higher cost than basic billing platforms.
Features:
- AI-native claims engine with advanced rules.
- Automated insurance verification from card images.
- Ambient note-taking and AI-driven coding.
Why It Stands Out:
- Access to large payer network data.
- Continuous learning from national benchmarks.
- High first-pass claim success rate.

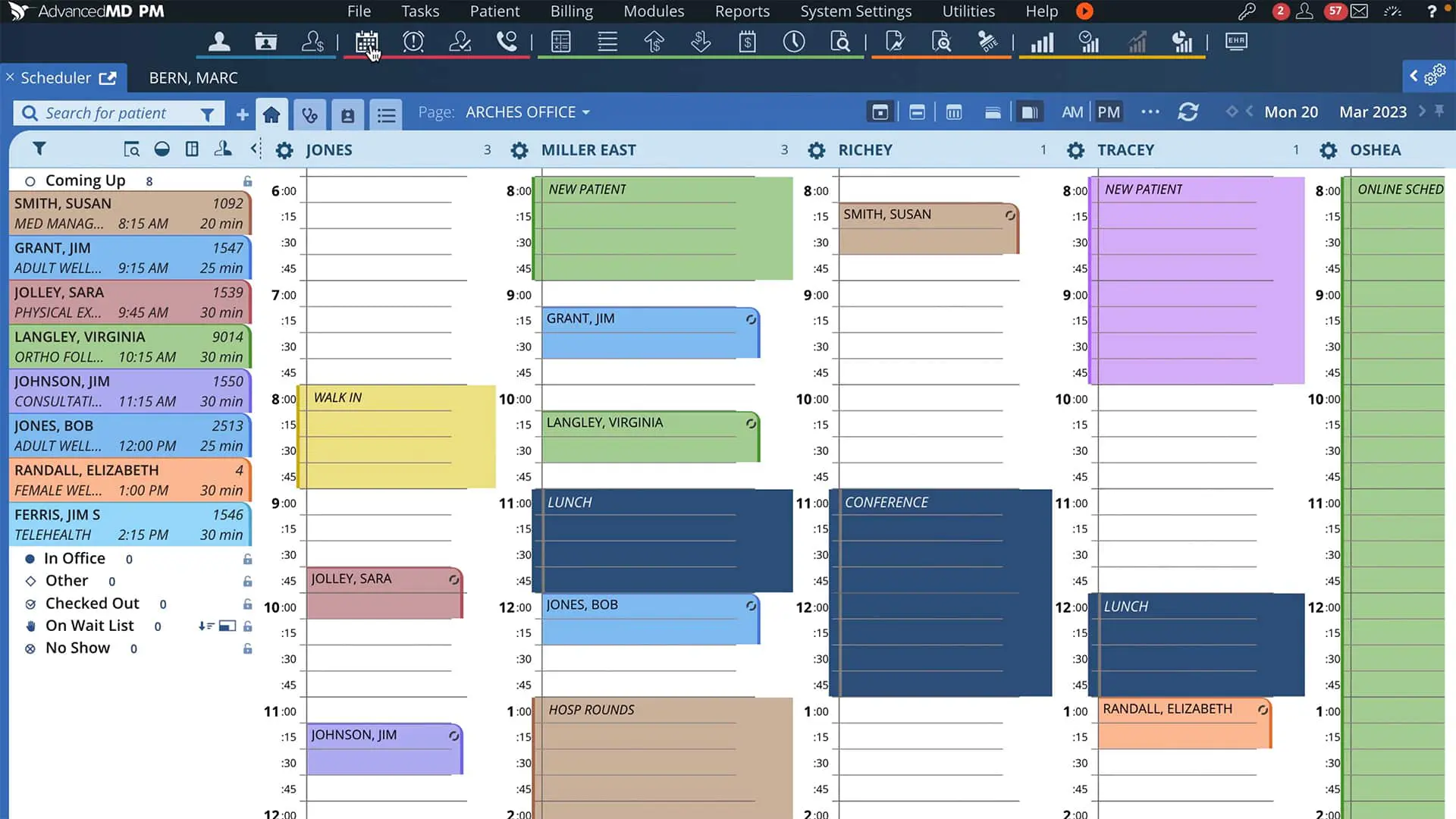
AdvancedMD, founded in 1999, provides cloud-based practice management, EHR, and medical billing solutions for healthcare organizations of all sizes. Their platform includes AI-driven tools for charge capture, denial management, and reporting to improve accuracy and revenue. AdvancedMD’s solutions help practices reduce stress on manual workload, driving patient satisfaction and supporting informed financial decision-making.
Software Interface
Pros:
- Strong analytics improve financial transparency.
- Automation reduces manual billing tasks.
- Scalable for both small and large practices.
Cons:
- Cost may be high for small practices.
- Onboarding time can be significant.
- Customization often requires technical support.
Features:
- Predictive analytics for billing and revenue.
- Automated denial resolution and re-submission workflow.
- Integrated patient billing and payment processing.
Why It Stands Out:
- All-in-one billing and EHR solution.
- Highly scalable for multi-location groups.
- Advanced AI analytics for decision-making.

Tebra has been providing billing solutions since 2003, supporting mid- and large-sized medical practices and billing companies. Their cloud-based EHR software streamlines administrative workflows and practice management. Tebra’s platform helps reduce billing errors, improve operational efficiency, and enhance patient care.
Software Interface
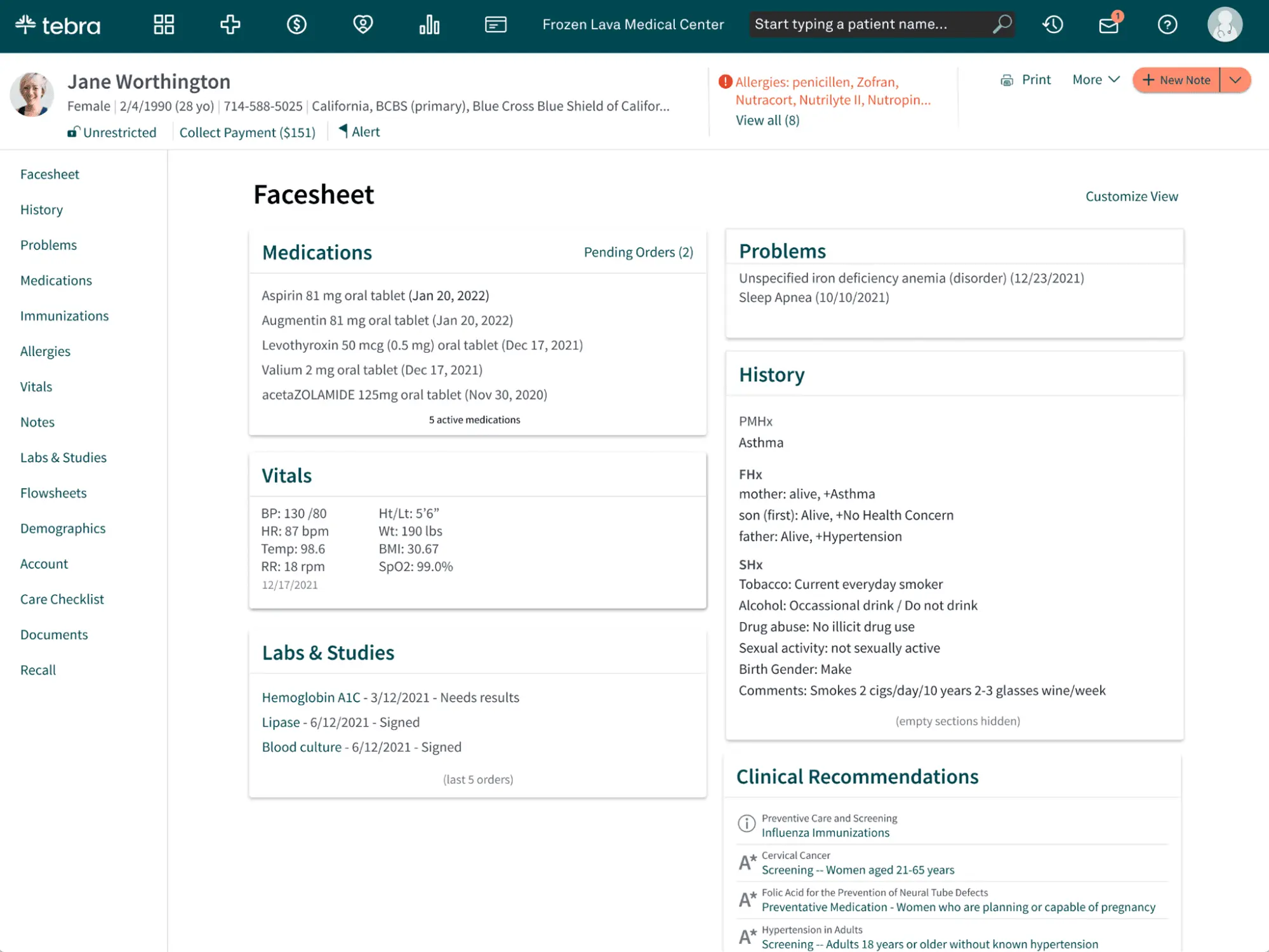
Pros:
- AI notes improve documentation accuracy.
- RPA automates repetitive billing tasks.
- EHR and billing are fully integrated.
Cons:
- Limited advanced enterprise analytics.
- May not scale easily for large health systems.
- UI can feel less configurable for complex workflows.
Features:
- RPA-driven claim scrubbing and eligibility checks.
- AI-powered note assistant for documentation and coding.
- Automatic claim submission and payment reconciliation.
Why It Stands Out:
- Streamlines patient-to-payment workflows.
- Merges billing and patient communication.
- Ideal for modern hybrid practices.

CureMD, headquartered at 80 Pine Street, 21st Floor, New York, NY, has been serving healthcare providers since 1997. They support a wide range of providers, from mid-sized practices to large hospitals, across multiple specialties. Their platform leverages AI-powered, cloud-based tools to streamline operations and improve care delivery.
Software Interface
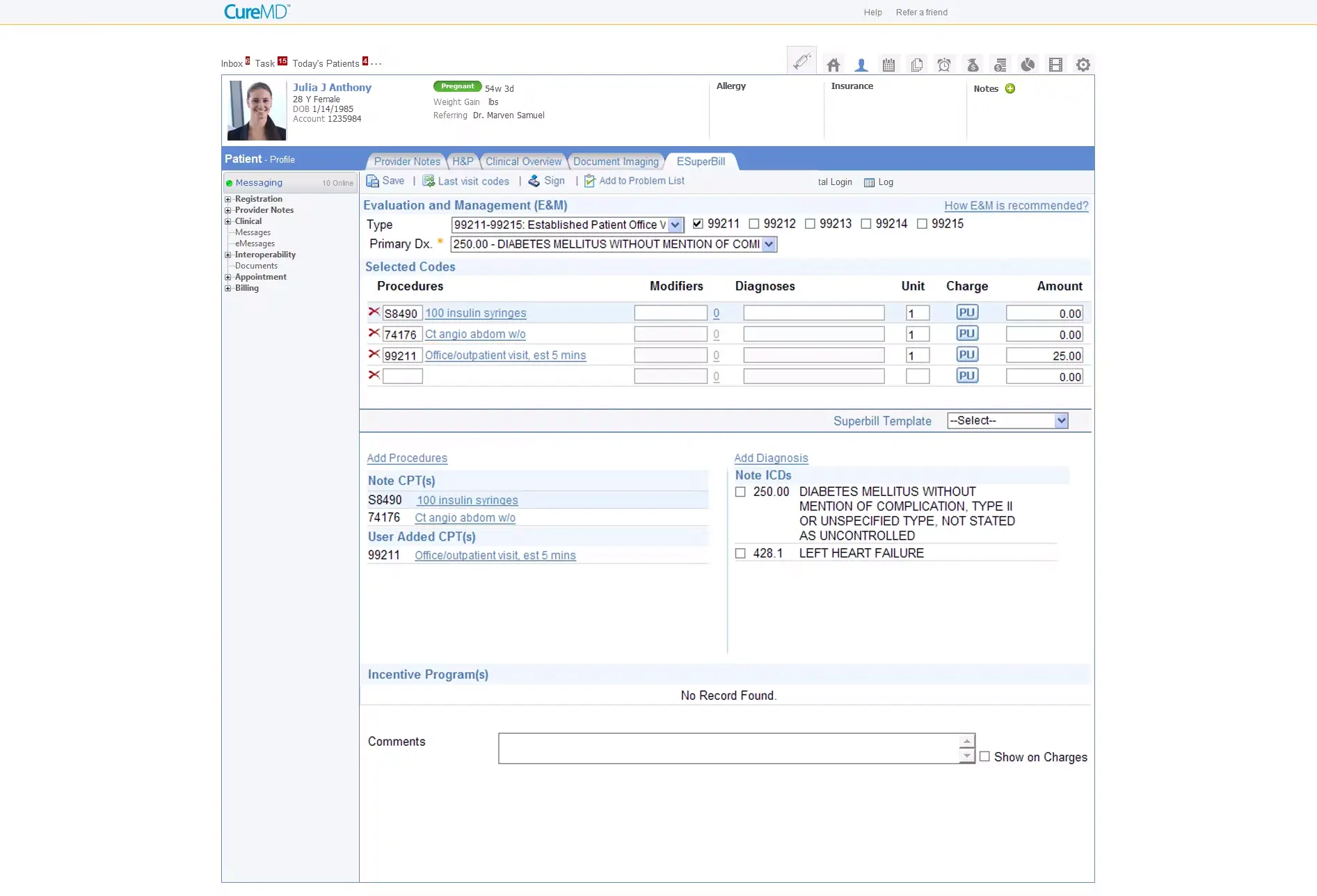
Pros:
- Automated billing boosts payment accuracy.
- Scalable platform for growing practices.
- Real-time dashboards provide financial clarity.
Cons:
- Onboarding can be complex for small practices.
- Pricing may not be transparent for all.
- Requires ongoing management to maximize benefits.
Features:
- Auto-claim scrubbing with built-in payer rules.
- Denial management and re-submission tools.
- Real-time analytics on cash flow and A/R.
Why It Stands Out:
- AI ensures error-free billing processes.
- Built-in compliance and audit tools.
- Great for multi-specialty medical groups.

Founded in 1999, CareCloud Inc. supports healthcare organizations of all sizes. Their cloud-based platform includes AI-powered Revenue Cycle Management (RCM), Electronic Health Records (EHR), Practice Management (PM), and Telehealth services. CareCloud also features CirrusAI, a suite of generative AI tools that automate clinical documentation.
Software Interface
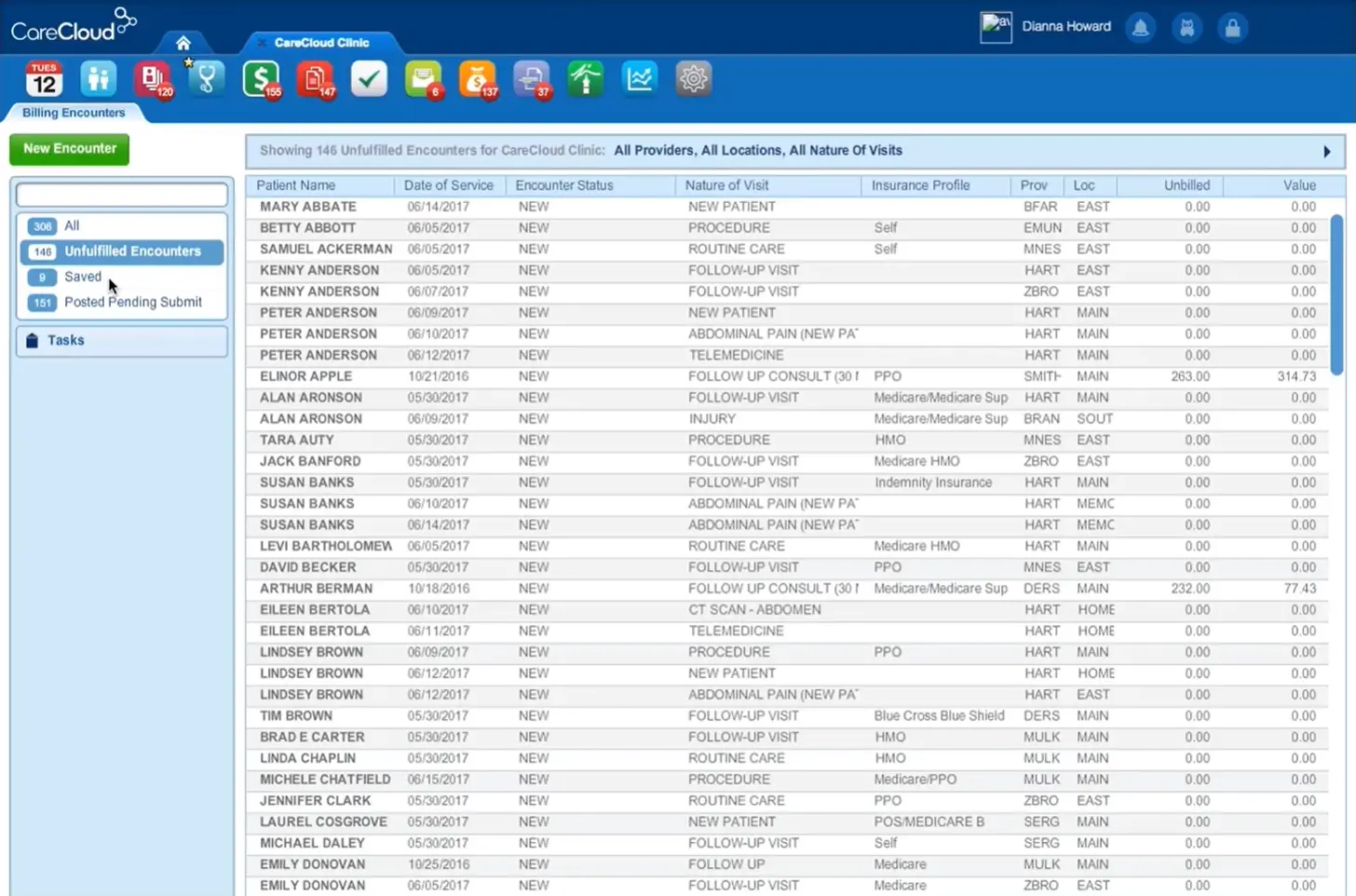
Pros:
- Real-time financial insights increase transparency.
- Automation minimizes manual billing errors.
- Unified interface supports cohesive workflows.
Cons:
- May require configuration for specialty workflows.
- Advanced analytics require additional training.
- Initial setup takes time for adoption.
Features:
- Real-time financial and billing dashboards.
- Automated billing rules to correct claim errors.
- Patient payment reconciliation and statements.
Why It Stands Out:
- AI predicts and prevents claim issues.
- Seamlessly integrates with EHR & PM software.
- Scalable, enterprise-grade performance.

NextGen Healthcare, established in 1974, provides comprehensive solutions for medical practices, hospitals, and large health systems. They serve a wide range of specialties, supporting both independent practices and enterprise-level organizations. Their platform includes EHR, practice management, and AI-powered billing tools.
Software Interface
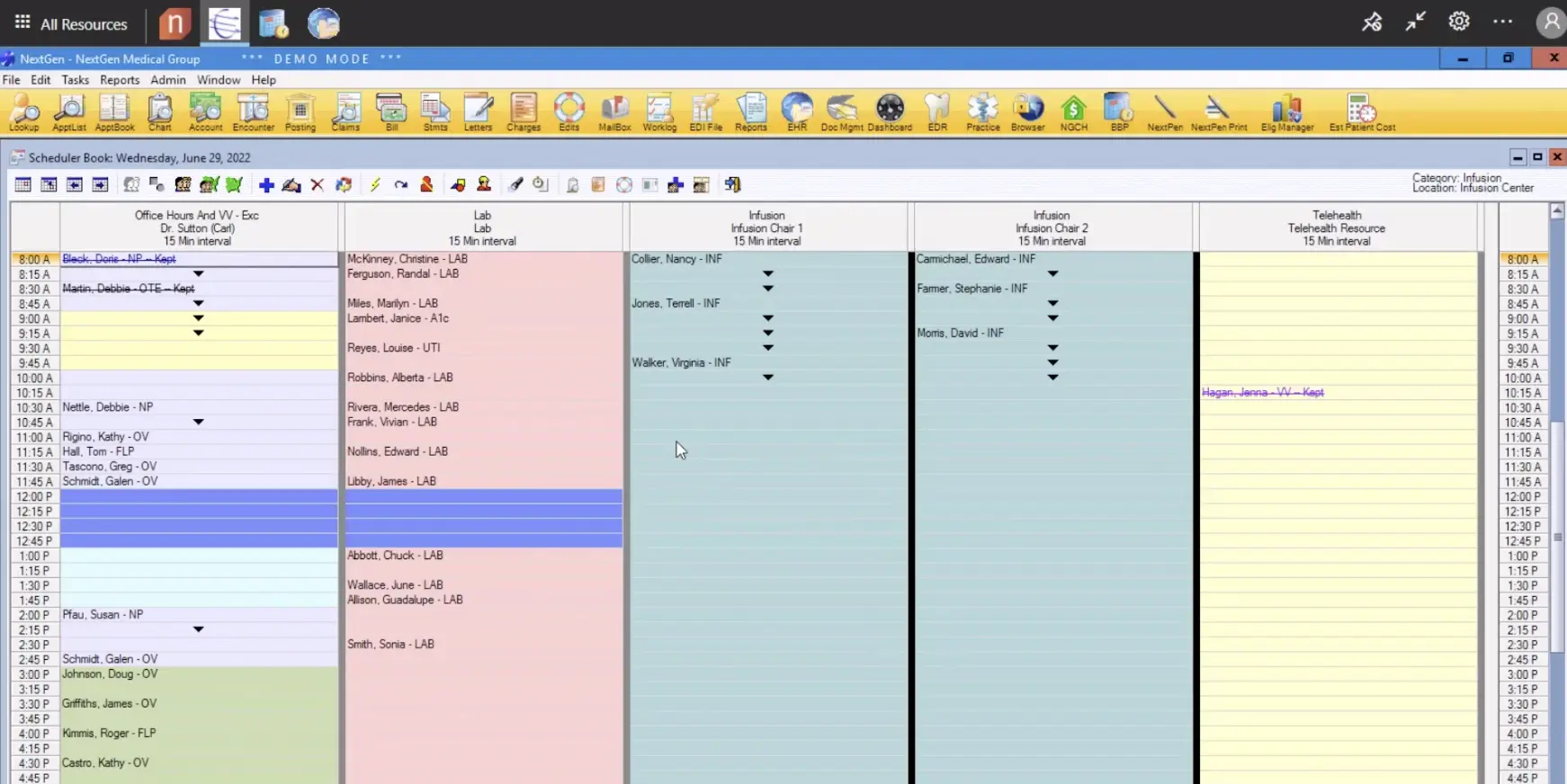
Pros:
- Automated charge review reduces billing errors.
- Specialty-specific rules support nuanced coding.
- Expert RCM team handles complex claims.
Cons:
- Needs training for rules engine use.
- Higher cost than basic billing platforms.
- Customization may require specialized implementation.
Features:
- Automated charge review rules engine.
- Specialty-specific coding and validation.
- Customizable analytics dashboards.
Why It Stands Out:
- Designed for mid-to-large healthcare systems.
- Reduces denials with predictive AI checks.
- Excellent reporting and compliance tools.

CollaborateMD, founded in 1999, provides cloud-based medical billing and practice management solutions for practices of all sizes. They serve a wide range of specialties, supporting independent providers, multi-provider practices, and medical billing companies. Their platform includes automated billing, reporting, and analytics tools.
Software Interface
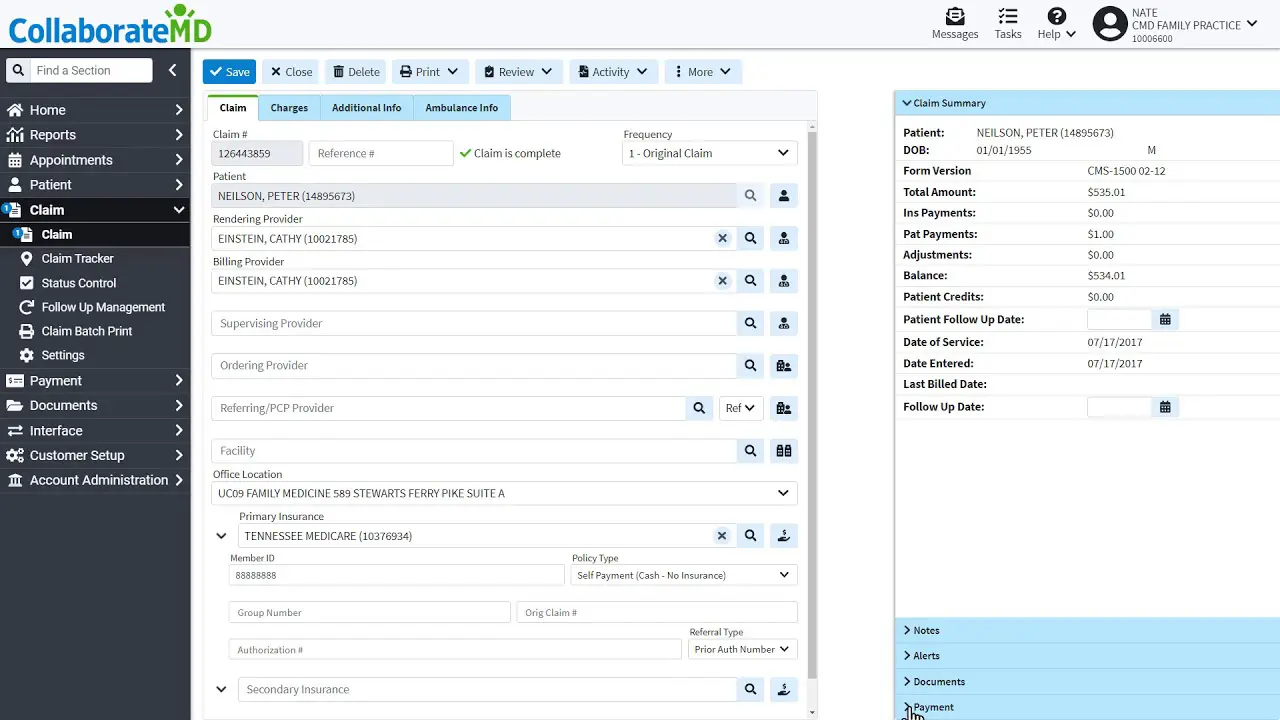
Pros:
- Web-based access supports remote teams.
- Automated eligibility verification reduces denials.
- Detailed reporting improves financial visibility.
Cons:
- Interface feels less modern than its competitors.
- Some advanced reporting is a paid upgrade.
- Learning curve for beginners.
Features:
- Automated eligibility checks and claim scrubbing.
- Remote web-based billing interface.
- Denial tracking and follow-up tools.
Why It Stands Out:
- Affordable and easy to implement.
- Fast, accurate claim submission process.
- Ideal for smaller or new practices.

RXNT, founded in 1999, offers cloud-based EHR, practice management, and medical billing solutions for healthcare providers of all sizes. They support a wide range of specialties, including independent practices and multi-provider groups. Their platform includes AI-powered tools for billing, scheduling, and patient management to improve accuracy and revenue performance.
Software Interface
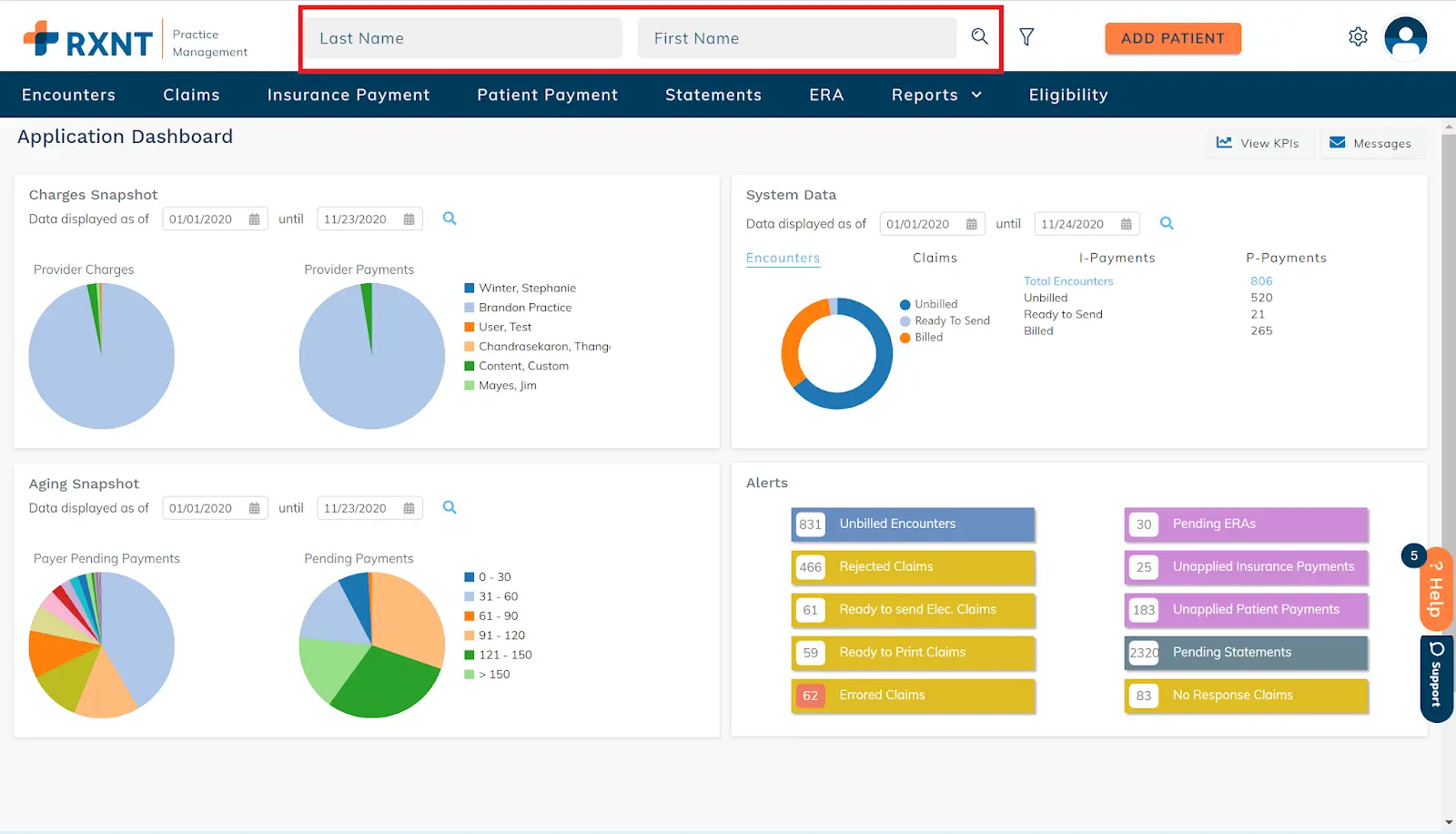
Pros:
- Intuitive system simplifies billing workflows.
- Real-time eligibility cuts payer surprises.
- Automation speeds claims and payments.
Cons:
- Less advanced analytics than enterprise solutions.
- Limited customization for niche specialties.
- May not scale to very large organizations.
Features:
- Real-time insurance eligibility verification.
- Automated claim submission and denial follow-up.
- Patient invoicing and payment processing.
Why It Stands Out:
- Affordable yet powerful billing suite.
- Excellent support and user training.
- Streamlined for small to mid-sized clinics.
Benefits of AI-Enabled Medical Billing Software
AI medical billing automates claims submission, speeding up the process by verifying patient data and reducing human error. It detects and corrects billing errors, such as incorrect coding or missing modifiers, before claims go out. Predictive analytics help flag high-risk claims and prioritize those likely to be denied. The software continuously adapts to regulatory changes, keeping billing compliant with payer rules. Overall, AI reduces operational costs, improves cash flow, and allows staff to focus on higher-value tasks.


What to Consider When Choosing an AI Medical Billing Software
When choosing a medical billing software, it’s essential to focus on integration, flexibility, and reliability. A platform like CureAR aligns with your workflow, scales with your growth, and maintains the highest security standards to protect patient data.
Continuous support and compliance are equally important for long-term success.
Key Considerations:
- Seamless integration with existing systems.
- Customizable to fit your workflow.
- Scalable for growing healthcare practices.
- Comprehensive support and staff training.
- HIPAA-compliant with strong data security.
Your Questions, Our Solutions
1. What is AI medical billing software?
The next generation of billing software uses artificial intelligence and automation to manage claims, detect coding errors, predict denials, and streamline revenue cycle operations. It helps healthcare providers improve accuracy, speed, and compliance in their billing process.
2. How does AI improve the billing process?
AI minimizes manual errors, automates claim submission, predicts denials, and adapts to payer rule changes in real time. This leads to faster reimbursements and fewer rejected claims.
3. Is AI billing suitable for small practices?
Yes. Many AI billing software are scalable and customizable, offering small practices automation tools without enterprise-level costs. They can also integrate with existing EHRs or practice management systems.
4. What features should I look for in medical billing software?
Look for features like predictive analytics, real-time claim scrubbing, EHR integration, compliance monitoring, denial management, and HIPAA-grade security.
5. How secure is AI-enabled billing software?
Reputable medical billing software providers use strong encryption, HIPAA compliance, and secure data hosting to ensure patient and financial information remains protected.

