Healthcare providers and billing teams are under growing pressure. Rising costs, staffing shortages, and complex insurance rules make managing claims a constant challenge. On average, hospitals lose around $5 million annually due to denied claims. In smaller practices, nearly 20% of claims are denied, and many are never resubmitted.
Manual billing consumes valuable time and increases errors, making it harder to maintain steady revenue and smooth operations. This is where medical billing software makes a difference. It manages the entire revenue cycle by automating tasks such as claim creation, insurance verification, coding, payment tracking, and reporting, thereby saving time and improving accuracy.
This guide will cover everything you need to know about medical billing software.
What is Medical Billing Software?
Medical billing software is a specialized system that helps healthcare providers manage the billing and reimbursement process with efficiency and accuracy.
- It automates key tasks like creating and submitting insurance claims, verifying patient information, tracking payments, and managing denials or rejections.
- By connecting with electronic health records (EHR) and practice management systems, the software ensures that patient data, diagnoses, and treatment details are correctly translated into standardized billing codes.
- Medical billing software also offers real-time reporting and analytics, giving providers insights into revenue trends, unpaid claims, and overall financial performance.
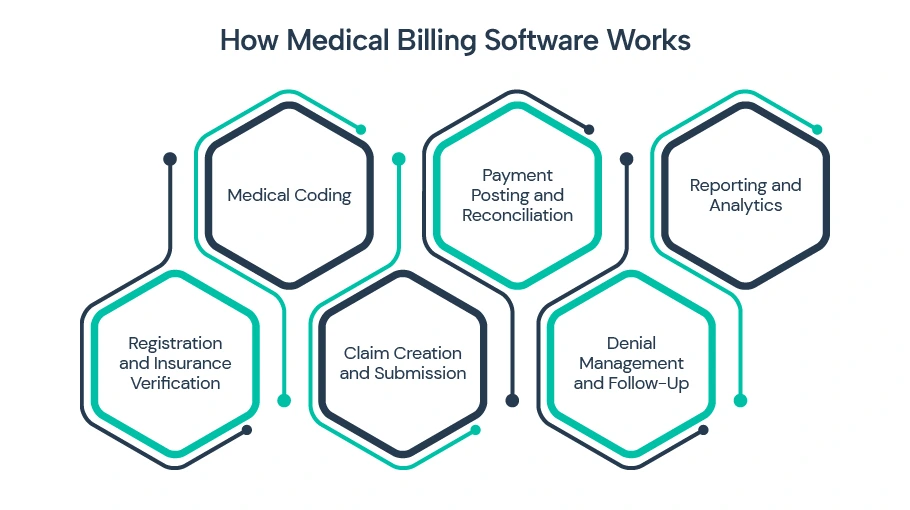
How Medical Billing Software Works
The workflow of billing software generally follows the Revenue Cycle Management (RCM) process, covering every stage from patient registration to final payment.
1: Registration and Insurance Verification
The process begins when patient information is entered into the system, including demographics, medical history, and insurance details. The software then verifies insurance eligibility in real time through payer portals or electronic verification tools.
2: Medical Coding
After services are provided, they must be translated into standardized codes for billing. Diagnoses are coded using ICD-10, while procedures use CPT or HCPCS codes. Advanced software often uses AI and Natural Language Processing (NLP) to extract relevant codes directly from clinical notes.
3: Claim Creation and Submission
Once coding is complete, the software generates claims in standard formats, such as ANSI X12 837, ready for electronic submission. Claims are then sent through clearinghouses, which validate the information and forward them to insurance companies.
4: Payment Posting and Reconciliation
After insurers process the claims, the software matches incoming payments to the correct patient accounts. It checks each payment against the claim details, identifies discrepancies, and flags them for review. The system can automatically adjust simple mismatches or route more complex issues to staff for verification.
5: Denial Management and Follow-Up
When a claim is denied, the software records the denial and identifies the reason using built-in rules and AI analysis. It can generate appeal forms, schedule follow-ups, and track communication with payers. Some systems also analyze patterns to prevent similar errors in future claims.
6: Reporting and Analytics
The software gathers data from all billing activities and organizes it into dashboards and reports. It analyzes claims, payments, and coding patterns using built-in analytics tools. Predictive models and automated reporting help staff monitor trends and prioritize workflow efficiently.
Tools and Technologies Used in Medical Billing Software
Modern billing software relies on several advanced tools and technologies.
- EHR Integration: Gathers clinical and patient data automatically.
- Clearinghouse Integration: Submits claims to multiple insurers electronically.
- Artificial Intelligence (AI): Suggests correct codes, predicts denials, and identifies errors.
- Natural Language Processing (NLP): Extracts relevant billing info from unstructured clinical notes.
- Automation Tools: Handle repetitive tasks like claim submission, reminders, and payment posting.
- Cloud-Based Platforms: Offer secure, scalable access and centralized data storage.
- Analytics & Reporting Tools: Track trends, revenue leakage, and performance metrics.
Benefits of Using Medical Billing Software
Using an advanced billing software offers more than just faster payments: it makes handling claims and billing a lot easier and less stressful.
Below, we’ve outlined the major benefits of using billing software.
1: Improved Accuracy and Fewer Errors
Billing software helps reduce common mistakes associated with manual processes. By automatically verifying patient information, insurance coverage, and medical codes, it spots errors before claims are submitted.
2: Faster Reimbursements and Better Cash Flow
Automated billing systems speed up the revenue cycle by improving claim submission and payment posting. This helps providers receive payments more quickly, improving cash flow and reducing the time staff spend chasing unpaid claims.
3: Time and Cost Efficiency
Repetitive tasks like claim generation, insurance verification, and follow-ups are handled automatically. Staff can focus on patient care instead of paperwork, and practices save on labor costs. Cloud-based medical billing software provides flexible, secure access from anywhere, making it easier for growing practices to scale.
4: Enhanced Compliance and Data Security
Billing solutions help practices stay compliant with regulations like HIPAA. Features such as secure storage, audit trails, and automated checks protect patient data and reduce the risk of fines or penalties.
5: Advanced Reporting and Insights
Dashboards and analytics tools allow practices to track revenue, claim status, and trends in real time. Predictive analytics can highlight at-risk claims and help optimize the revenue cycle, enabling smarter business decisions.
6: Flexibility for Different Practice Sizes
Whether running a small clinic or a large hospital, medical billing software scales to meet the practice’s needs. Practices can also outsource medical billing services, combining software automation with expert support to expand efficiency and revenue.
Common Challenges Faced by Providers and How Billing Software Solves Them
Managing billing in healthcare is complex, and providers face several challenges that can affect both revenue and operations. Advanced billing software addresses these issues effectively, making the process smoother and more accurate.
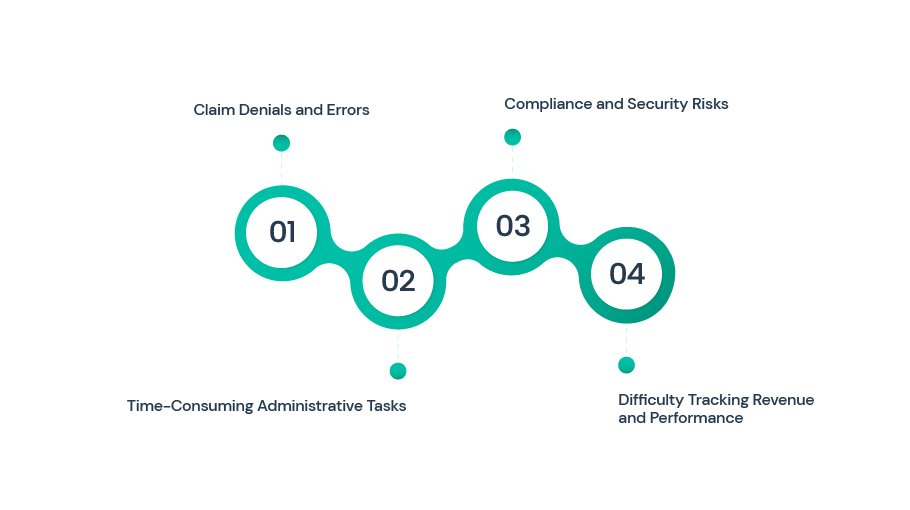
1: Claim Denials and Errors
One of the biggest headaches for providers is claim denials, often caused by incorrect codes, missing information, or insurance mismatches. Denials not only delay payments but also require staff to spend extra time on corrections.
Medica billing software tackles this with automated coding tools and real-time claim validation. These tools verify ICD-10, CPT, and HCPCS codes before claims are submitted and check patient insurance eligibility. Some advanced systems even use AI-powered algorithms to predict potential denials.
2: Time-Consuming Administrative Tasks
Manual billing involves repetitive work such as entering patient information, generating claims, and following up on unpaid invoices. This consumes valuable time and increases the risk of human error.
Automation features in software simplify these tasks. Tools like automated payment posting and workflow management systems handle repetitive processes, ensuring claims are submitted, payments are tracked, and follow-ups are scheduled automatically.
3: Compliance and Security Risks
Medical billing software must comply with regulations such as HIPAA and payer-specific guidelines. Manual processes can make it hard to maintain consistent compliance and secure patient data.
The software includes built-in compliance checks and secure data storage, protecting sensitive information and providing audit trails for every transaction. This reduces the risk of fines, penalties, or data breaches.
4: Difficulty Tracking Revenue and Performance
Without proper tools, it’s challenging to monitor unpaid claims, denials, or overall revenue trends. Practices may lose sight of important financial metrics.
Reporting and analytics features within software give a real-time overview of revenue cycles, claim status, and staff performance. Predictive analytics can highlight patterns, such as recurring denial reasons or delayed payments.
Medical Billing Software for Different Practice Sizes
The global medical billing software market, valued at $16.34 billion in 2023 and projected to reach $32.18 billion by 2030 at a CAGR of 10.2%, demonstrates the increasing adoption of these solutions across healthcare organizations. This growth shows that providers of all sizes are turning to software to manage billing more efficiently. However, medical billing needs still vary depending on practice size. A small clinic has different demands than a multi-specialty hospital.
Small Practices
For small clinics, resources are often limited, and staff wear multiple hats. Manual billing can be time-consuming and error-prone. Medical billing software for small practices helps automate claim submissions, insurance verification, and payment posting, reducing the administrative burden. Cloud-based solutions are especially beneficial for small practices, offering secure access without the need for extensive IT infrastructure.
Medium-Sized Practices
Medium-sized practices typically manage higher patient volumes and more complex billing scenarios. Software supports these practices by integrating with EHR systems, providing analytics dashboards, and automating denial management.
Large Hospitals and Multi-Specialty Centers
Large healthcare organizations handle thousands of claims and work with multiple insurance providers every day. Advanced billing software supports these organizations by automating workflows across departments and simplifying complex billing processes.
Conclusion
Medical billing software is essential for healthcare providers of all sizes. It automates key tasks such as claim submission, coding, insurance verification, and payment tracking, reducing errors and accelerating reimbursements. Automation also frees staff to focus on patient care instead of administrative work.
Advanced tools like AI, predictive analytics, and workflow automation help practices identify potential claim denials and address them proactively. Scalable solutions adapt to any practice size, ensuring accurate billing, streamlined operations, and improved revenue management. These systems simplify complex processes and support consistent, efficient financial operations across the healthcare industry.
Frequently Asked Questions
Medical billing software is a digital tool that automates the billing process for healthcare providers, including claim creation, coding, insurance verification, and payment tracking.
It follows the revenue cycle management process, from patient registration and coding to claim submission, payment posting, and reporting, often using AI and automation to reduce errors.
Yes, most solutions integrate with EHR/EMR systems, clearinghouses, and analytics platforms to improve workflows and maintain accurate patient and financial data.
Absolutely, Small businesses and billing companies can automate repetitive tasks, manage claims efficiently, and scale operations without increasing staff or costs.
Yes, it uses encryption, access controls, and audit trails to protect patient data and meet HIPAA requirements.








